[av_heading heading=’Total Knee Replacement (Knee Arthroplasty)’ tag=’h3′ style=” subheading_active=” show_icon=” icon=’ue800′ font=’entypo-fontello’ size=” av-medium-font-size-title=” av-small-font-size-title=” av-mini-font-size-title=” subheading_size=” av-medium-font-size=” av-small-font-size=” av-mini-font-size=” icon_size=” av-medium-font-size-1=” av-small-font-size-1=” av-mini-font-size-1=” color=” custom_font=” subheading_color=” seperator_color=” icon_color=” margin=” margin_sync=’true’ padding=’10’ icon_padding=’10’ headline_padding=” headline_padding_sync=’true’ link=” link_target=” id=” custom_class=” template_class=” av_uid=’av-ktt49gp1′ sc_version=’1.0′ admin_preview_bg=”][/av_heading]
[av_textblock size=” av-medium-font-size=” av-small-font-size=” av-mini-font-size=” font_color=” color=” av-desktop-hide=” av-medium-hide=” av-small-hide=” av-mini-hide=” id=” custom_class=” template_class=” av_uid=” sc_version=’1.0′]
A total knee replacement (TKR) or total knee arthroplasty is a surgery that resurfaces an arthritic knee joint with artificial metal or plastic replacement parts called the ‘prostheses’.
Doctors may recommend surgery for people suffering from severe arthritis in the knee to decrease the pain and to improve the patient’s ability to walk.
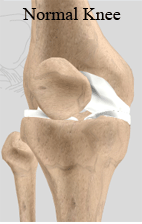
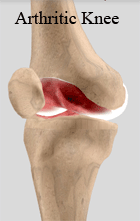
In an arthritic knee
- The cartilage lining is thinner than normal or completely absent. The degree of cartilage damage and inflammation varies with the type and stage of arthritis.
- The capsule of the arthritic knee is swollen
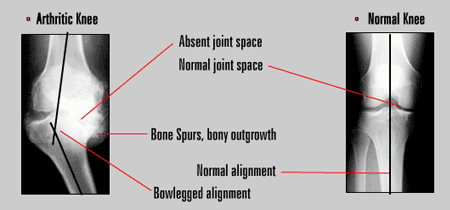
- The joint space is narrowed and irregular in outline; this can be seen in an X-ray image.
- Bone spurs or excessive bone can also build up around the edges of the joint.
The combinations of these factors make the arthritic knee stiff and limit activities due to pain or fatigue.
Diagnosis
- The diagnosis of osteoarthritis is made on history, physical examination & X-rays
- There is no blood test to diagnose Osteoarthritis (wear & tear arthritis)
Total knee replacement procedure
A longitudinal skin incision is made down the front of your knee. This incision usually measures around 15cm. The kneecap is reflected out of the way and the arthritic surfaces are removed. Soft tissue releases are performed. Special instrumentation is used to remove the bone in a specified manner so that a knee replacement prosthesis can fit onto the bone with or without cement.
Some prostheses do not require cement fixation and the bone grows into them. Other prostheses require cement fixation. Your surgeon will decide which is the best fixation prosthesis for your quality bone. Once the two metal components are fixed to the bone, a plastic insert is placed on the tibial surface. This plastic acts as the shock absorber. The plastic allows the low friction movement to occur. The plastic may either be fixed or mobile depending on the type of prosthesis.
The kneecap may also require resurfacing depending on the amount of wear. This is done by removing half the under-surface of the kneecap (patella) and cementing a plastic kneecap in its place.
Soft tissue releases are performed to balance the knee joint and after the prosthesis has been placed in the knee, the knee should appear straight and flex to over 110 degrees.
Many arthritic knees are bowed due to the arthritis. A total knee replacement will correct this mal-alignment. Some knees are knock-kneed and similarly the replacement will correct the mal-alignment. Following the surgery the wound is closed with absorbable sutures and a drain is inserted.
Post-operative physiotherapy is started after 24 to 48 hours. It is important to do all the exercises as they will allow a quicker recovery. Quadriceps exercises and knee extension and flexion exercises are most important. You should expect to gain a range of motion from 0 to 110 degrees. Very stiff knees often do not regain this amount of movement. Knees that start off with 140 degrees of movement may lose approximately 20 degrees of movement following the replacement.
Complications Anesthesia complications
As anybody undergoes general or regional anesthesia (epidural anesthesia) there are always risks associated with it. The risks of course are magnified if you have abnormal general medical conditions in addition to your older age, which may have affected the functions of your vital organs such as heart, lungs and kidneys. Therefore a complete evaluation of those systems has to be performed before you are taken to the Operating theatre.
Specific complications relating to knee replacement surgery include the following
-
- Deep vein thrombosis The risk of this occurring is lowered by giving blood thinning medication. However if it does occur more specific treatment is given.
-
- Infection The risk of infection is less than 1% and pre-operative antibiotics are given to prevent this from happening.
-
- Stiffness Occasionally knee replacement may stiffen up particularly in patients who are significantly overweight or have diabetes. Occasionally one will require a manipulation under an anaesthetic should this occur.
-
- Nerve and vessel damage It is unlikely that any major nerve or vessel will be damaged. It is, however, very common to have a small area of numbness over the outer side of your knee where a superficial skin nerve is always cut during the surgery. This little numb patch is of no significance.
-
- Prosthesis failure The prosthesis may fail due to the plastic wearing out and it may require revision.
-
- Reflex sympathetic dystrophy Very rarely a condition can occur where the leg becomes stiff, hypersensitive and painful. This requires specific treatment with a pain management specialist.
-
- Excessive bleeding around the joint This usually settles but may require drainage.
-
- Excessive scarring Some skin will scar up significantly (keloid).
-
- Fluid build-up in the knee joint Occasionally this may occur and require drainage. It is usual for knees to be a little swollen and a little warm.
-
- Pain with kneeling Kneeling may produce discomfort over the incision site.
A total knee replacement often takes at least six months to settle in.